HEALTH
From Flat Rates to Percentages: Billing Explained

Choosing the right billing model is a critical step in managing the financial health of your medical practice. With various options available, the debate between flat rate and percentage-based billing continues to be relevant. Understanding how each model operates and what it means for your bottom line helps you make informed decisions. If you’re evaluating your options and considering what fits your budget best, exploring Medical Billing Services Pricing is a good place to start. Here’s a breakdown of how each model works and which could be the better fit for your unique needs.
Understanding Flat Rate Billing
Flat rate billing is exactly what it sounds like: a fixed, predictable fee charged monthly or per service, regardless of how much revenue your practice generates or how many claims are processed. This model is favored by practices that prefer consistency in budgeting and value simplicity over flexibility.
With flat rate billing, you typically agree to a predetermined monthly fee with your medical billing provider. This fee may be based on the size of your practice, volume of claims, or types of services offered. Whether you process 200 or 500 claims in a month, the fee remains the same.
Advantages of Flat Rate Billing
- Predictable monthly expenses
- Simplified budgeting
- Easier to compare service costs across vendors
- No surprises with rising collections
Disadvantages of Flat Rate Billing
- May cost more during slow months
- Less flexible to scale with growing practices
- Potential risk of overpaying for low-volume periods
This model tends to work best for small to medium-sized practices that have steady claim volumes and want to avoid fluctuations in costs.
What Is Percentage-Based Billing?
Percentage-based billing is a model where the billing company charges a percentage of the total collections. This means the provider earns more when your practice collects more, aligning incentives between the billing company and your revenue performance.
Typically, the percentage charged ranges between 4% and 9% of the collected revenue, depending on the specialty, claim volume, and complexity of billing processes.
Advantages of Percentage-Based Billing
- Aligns provider’s revenue with billing performance
- Lower costs during slower months
- Flexible and scalable as the practice grows
- Motivates billing company to collect efficiently
Disadvantages of Percentage-Based Billing
- Harder to predict monthly costs
- Risk of paying more during high-volume months
- Requires careful auditing to ensure accuracy in collections
This model is generally more attractive to larger or rapidly growing practices where scalability and performance-based incentives are a priority.
Comparing Cost Efficiency
The real difference between flat rate and percentage billing lies in cost-efficiency and alignment of goals.
Let’s say a practice collects $100,000 in a given month. Under a percentage model at 6%, the billing cost would be $6,000. Compare that to a flat fee of $4,000/month, and the flat rate seems more cost-effective—unless the practice’s collections dip below $66,000, in which case the percentage model becomes cheaper.
Ultimately, the better model depends on claim volume, consistency in revenue, and how much variability your practice is comfortable managing.
Which Model Is Best for Your Practice?
To choose between flat rate and percentage billing, consider the following:
- Is your claim volume steady or seasonal?
- Do you want consistent monthly expenses or performance-based flexibility?
- Can you manage the administrative oversight required to audit a percentage-based model?
If you’re running a small practice with predictable revenue and limited administrative support, a flat fee may offer peace of mind and simplicity. However, if you’re scaling rapidly or need your billing team to be more invested in collections, a percentage-based model may better serve your goals.
Hybrid and Custom Billing Structures
Some billing providers now offer hybrid models that combine the predictability of flat fees with the performance-driven aspects of percentage billing. For example, a base flat fee may be charged along with a smaller percentage of collections once a certain revenue threshold is surpassed.
This can help balance stability with performance incentives, especially for growing practices or those with fluctuating claim volumes. These custom arrangements allow for more negotiation and tailored agreements between the practice and the billing company.
Hidden Costs and Fine Print
Regardless of which model you choose, it’s essential to read the fine print in your billing service contract. Some providers add setup fees, EHR integration costs, reporting fees, or charges for reworking denied claims. These can inflate your actual cost significantly.
Always ask for a detailed breakdown of what’s included in the pricing and what services come with an additional fee. Flat rates may appear low but might not include advanced services like appeals management, credentialing, or analytics.
And remember that even percentage-based models can include minimum billing thresholds or require a commitment to a certain claim volume.
Real-World Example
A general practitioner’s office collecting about $80,000 monthly opted for flat rate billing at $4,200 per month. While this cost slightly more than the 5% percentage model they were considering, the consistent expense helped them plan their finances more easily, and the included services like denial management made it worthwhile.
On the flip side, a specialty surgical clinic with more variability in claims collection chose a 6.5% percentage billing model. This ensured that during slower months, their costs stayed lower, and their billing provider had the motivation to maximize collections.
One of their staff jokingly said they’d never heard of Medi-Solutions Management until they helped them recover six months of aging AR—worth every penny.
Final Thoughts
There is no one-size-fits-all answer to the flat rate vs. percentage billing debate. It all comes down to your practice’s size, revenue stability, and comfort with variable costs. A well-negotiated contract, clear understanding of included services, and regular performance reviews with your billing provider will go a long way toward ensuring you get value for your money.
Always take the time to assess your needs thoroughly, and don’t be afraid to ask providers to walk you through a sample invoice or simulation based on your current revenue data. The more informed you are, the better your billing strategy will support your long-term growth.
HEALTH
Attrities: Understanding the Condition, Symptoms, and Management
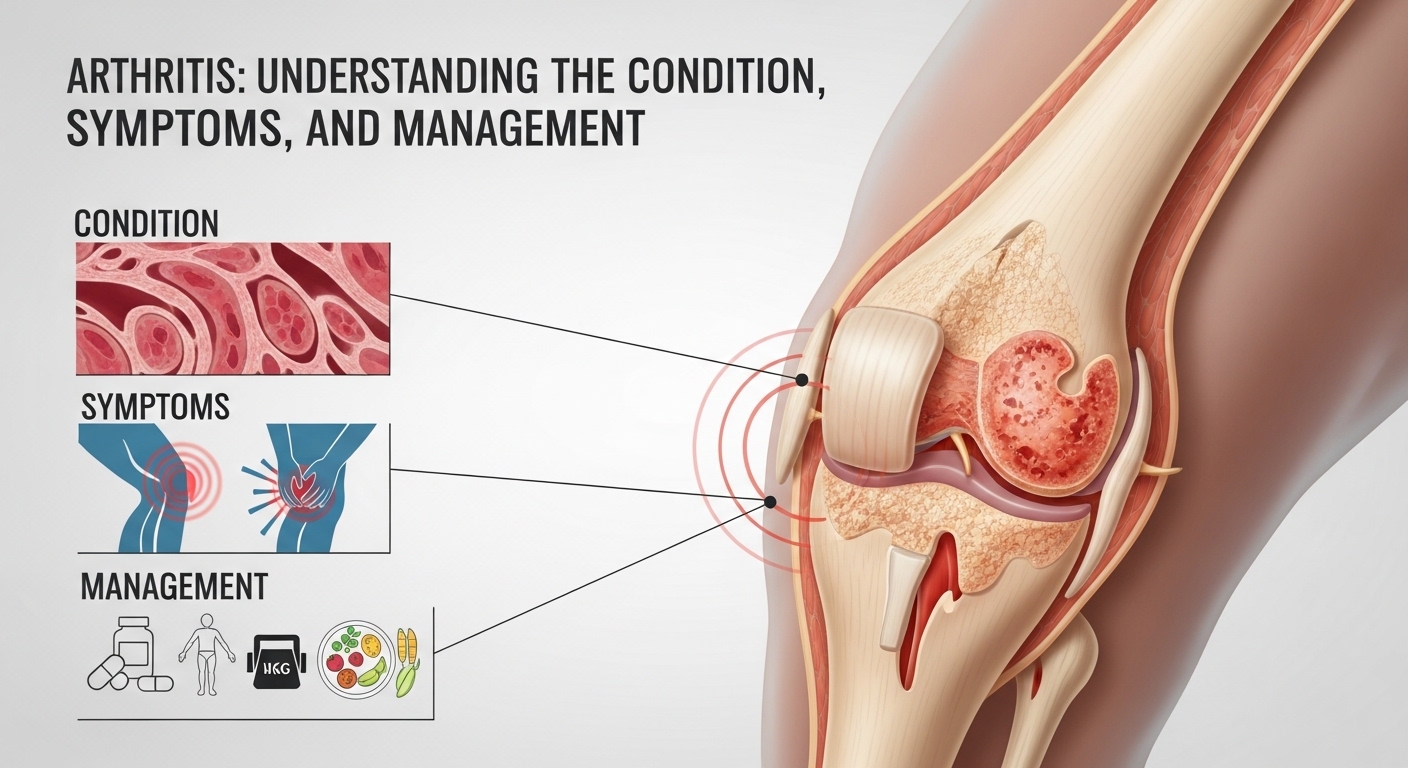
Attrities is a term often encountered in discussions about health, particularly relating to joint discomfort and mobility issues. While the term may sometimes be confused with attrition in organizational or military contexts, in medical usage, it is closely associated with arthritis—a common condition that affects millions worldwide. This article explores Attrities in depth, covering its causes, types, symptoms, and management options to provide a comprehensive professional overview.
What Are Attrities?
In the medical context, Attrities is most likely a reference to arthritis, a condition characterized by inflammation of the joints. Arthritis can affect people of all ages, though it is more common in older adults. The condition results in joint pain, stiffness, swelling, and decreased mobility, which can significantly impact daily activities and quality of life.
There are over 100 types of arthritis, ranging from osteoarthritis, which occurs due to wear-and-tear of cartilage, to rheumatoid arthritis, an autoimmune disorder where the immune system attacks joint tissues. Despite variations in cause and severity, the common thread among all forms of arthritis is joint dysfunction and discomfort. Understanding Attrities as arthritis emphasizes the need for early recognition and effective management to prevent long-term damage.
Causes of Attrities
The causes of Attrities vary depending on the type of arthritis. Osteoarthritis, the most common form, is typically caused by aging, joint injury, or repetitive stress on the joints. Genetics and obesity also play significant roles in increasing susceptibility to this condition.
Rheumatoid arthritis, on the other hand, is an autoimmune disorder where the immune system mistakenly targets the lining of the joints, causing inflammation and joint deformity over time. Other forms of Attrities may result from infections, metabolic issues like gout, or chronic inflammatory conditions. Identifying the specific cause is crucial for effective treatment planning.
Symptoms of Attrities
Symptoms of Attrities often develop gradually but can sometimes appear suddenly. Key signs include joint pain, tenderness, swelling, and stiffness, particularly in the morning or after periods of inactivity. In advanced cases, patients may experience reduced range of motion, joint deformities, and chronic fatigue.
Different types of arthritis may also present unique symptoms. For example, rheumatoid arthritis commonly affects symmetrical joints, whereas osteoarthritis often impacts weight-bearing joints like the knees and hips. Recognizing these patterns is vital for accurate diagnosis and timely intervention.
Diagnosis and Medical Assessment
Diagnosing Attrities involves a combination of physical examination, medical history, and imaging tests. Doctors often use X-rays, MRI scans, or ultrasound to assess joint damage and inflammation. Blood tests may also help identify autoimmune forms of arthritis, such as rheumatoid arthritis or lupus-related joint conditions.
Early diagnosis of Attrities is critical to slowing disease progression and reducing long-term joint damage. Healthcare providers emphasize monitoring symptoms and seeking medical evaluation if joint discomfort persists for more than a few weeks.
Treatment and Management Options
Managing Attrities typically involves a multi-faceted approach tailored to the type and severity of arthritis. Medications play a central role, including anti-inflammatory drugs, pain relievers, corticosteroids, or disease-modifying antirheumatic drugs (DMARDs) for autoimmune forms.
Lifestyle modifications are equally important. Regular exercise helps maintain joint mobility and muscle strength, while a balanced diet can support overall health and reduce inflammation. In severe cases, surgical interventions such as joint replacement may be necessary to restore function and relieve pain. Combining medical, physical, and lifestyle strategies is often the most effective way to manage Attrities.
Alternative Interpretation: Attrition
While the medical interpretation of Attrities relates to arthritis, the term may also be mistakenly used in organizational or military contexts, referring to attrition. In this sense, attrition describes the gradual loss of people from a program, workforce, or recruitment process. For example, military recruits dropping out during training could be described as attrition.
Though distinct from arthritis, this interpretation highlights the importance of context when using the term Attrities, ensuring clarity whether discussing health or organizational metrics.
Preventive Measures
Preventing Attrities in the arthritis sense focuses on protecting joint health and maintaining overall well-being. Regular physical activity, weight management, ergonomic adjustments, and avoiding repetitive joint stress can reduce the risk or severity of arthritis.
Early detection of symptoms also allows for prompt intervention, which can prevent complications such as chronic pain or reduced mobility. In high-risk individuals, routine check-ups and proactive lifestyle modifications can be particularly beneficial.
Living with Attrities
Living with Attrities requires ongoing attention to joint health and pain management. Patients are encouraged to develop a comprehensive care plan with healthcare providers, incorporating medication, exercise, and dietary strategies. Support groups and educational resources can also provide emotional and practical assistance.
Maintaining an active lifestyle, while respecting joint limitations, is essential. Adaptive techniques and assistive devices may further improve independence and quality of life for those affected by arthritis-related Attrities.
Conclusion
Attrities, most commonly associated with arthritis, represents a significant health concern affecting millions worldwide. By understanding its causes, symptoms, and treatment options, individuals can take proactive steps to manage the condition effectively. While occasionally confused with organizational attrition, the medical interpretation emphasizes the importance of joint care, early intervention, and holistic management strategies.
Recognizing and addressing Attrities empowers patients to maintain mobility, reduce pain, and enhance quality of life, making awareness and education critical components of health management.
HEALTH
Kill Tooth Pain Nerve in 3 Seconds Permanently? What You Really Need to Know
In today’s fast-paced world, dental pain feels unbearable, and it’s no surprise many people search online for ways to “kill tooth pain nerve in 3 seconds permanently.” Severe toothaches disrupt work, sleep, and overall quality of life. But can you truly end the pain instantly and permanently at home? The short answer is no—yet there are safe, effective ways to get relief and achieve a lasting solution.
This article explores what causes tooth nerve pain, why “quick fixes” are risky, and the proven options for permanent relief.
Understanding Tooth Nerve Pain
At the core of every tooth lies the pulp, which contains blood vessels and nerves. When bacteria or trauma inflame this pulp, the resulting pain can be intense. Common causes include:
-
Deep cavities exposing the nerve
-
Cracks or fractures reaching the pulp
-
Infections under the tooth (abscesses)
-
Gum disease exposing root surfaces
Because the nerve is living tissue, there is no safe at-home method to destroy it “in 3 seconds.” Only professional dental treatment can remove or treat a tooth nerve properly.
Why People Search “Kill Tooth Pain Nerve in 3 Seconds Permanently”
The phrase itself reveals the desperation many feel when experiencing a severe toothache. People want:
-
Immediate relief from unbearable pain
-
Permanent solutions so the pain won’t return
-
Low-cost or at-home remedies to avoid dentist visits
While the urgency is understandable, quick fixes often worsen the problem. Unverified online “hacks” involving chemicals, extreme temperatures, or sharp tools can cause infection, tissue damage, and even life-threatening complications.
Safe Ways to Manage Tooth Pain Temporarily
Although you can’t “kill” a tooth nerve at home, you can reduce pain until you see a dentist:
-
Over-the-counter pain relievers (ibuprofen or acetaminophen) as directed.
-
Cold compresses on the outside of the cheek to reduce swelling.
-
Saltwater rinses to help clean the area and soothe inflamed tissue.
-
Topical anesthetic gels containing benzocaine (used sparingly).
-
Elevating your head at night to reduce blood pressure in the area.
These measures don’t fix the underlying problem but can help you cope until you reach professional care.
Professional Treatments That Permanently Eliminate Tooth Nerve Pain
Dentists have several procedures to permanently stop nerve pain:
-
Root Canal Therapy (RCT): Removes infected pulp and seals the tooth. This is the most common permanent solution while keeping the tooth intact.
-
Extraction: If a tooth is beyond repair, removing it eliminates the nerve and the source of pain.
-
Pulp Capping or Partial Pulpotomy: In some cases, the dentist treats only part of the pulp to preserve tooth vitality.
-
Antibiotics: Used when infection spreads beyond the tooth, but always in combination with a definitive procedure.
These treatments are performed under local anesthesia, so you won’t feel pain during the procedure—and once completed, the source of the nerve pain is permanently resolved.
Why Permanent Relief Requires Professional Care
Attempting to “kill” a tooth nerve without dental training is dangerous. Risks include:
-
Infection spreading to the jaw or bloodstream
-
Damage to surrounding teeth or tissues
-
Uncontrolled bleeding or nerve injury
-
Delayed diagnosis of serious conditions (like abscesses or tumors)
Dentists use sterile techniques, precision instruments, and X-rays to ensure proper treatment and safe healing.
Modern Dentistry Makes Treatment Quick and Comfortable
One reason people search for “3 second” solutions is fear of the dentist. But modern dentistry offers:
-
Fast pain relief with local anesthetics and sedation options
-
Digital imaging for accurate diagnosis
-
Minimally invasive tools that shorten appointment times
-
Payment plans or insurance coverage to ease financial stress
Most patients find that once they’re numbed, treatment is far less painful—and far faster—than they feared.
Preventing Future Tooth Nerve Pain
Prevention remains the best strategy. You can minimize the risk of severe toothaches by:
-
Brushing twice daily with fluoride toothpaste
-
Flossing once a day to prevent gum disease
-
Limiting sugary foods and drinks
-
Visiting your dentist every 6 months for checkups
-
Addressing small cavities early before they reach the nerve
By maintaining oral health, you reduce the chances of ever needing emergency dental care.
The Role of Emergency Dentists
If you’re in severe pain outside normal office hours, search for an emergency dentist. Many offer same-day appointments, after-hours care, or on-call services. Immediate professional attention not only relieves pain but can save the tooth.
Looking Ahead: Advances in Dental Pain Management
Research into regenerative dentistry, pulp therapy, and biomaterials is ongoing. In the future, dentists may be able to heal tooth nerves instead of removing them. Until then, root canals and extractions remain the gold standard for permanent relief.
The Takeaway
While it’s tempting to believe there’s a way to “kill tooth pain nerve in 3 seconds permanently,” the reality is that only a dentist can safely remove or treat a tooth nerve. Home remedies can temporarily ease discomfort, but they cannot fix the root cause.
Modern dentistry makes permanent pain relief achievable, comfortable, and far faster than most people expect. Don’t risk your health with unverified shortcuts—seek professional care to end tooth pain for good.
HEALTH
Dog Stung by Bee: Understanding, Responding, and Preventing Future Incidents

In today’s fast-moving world where pets are part of the family, dog owners face all kinds of unexpected challenges. One common yet often misunderstood emergency is when a dog is stung by a bee. Just like people, dogs can experience anything from mild irritation to severe allergic reactions after a sting. Understanding how to respond quickly and appropriately can make the difference between a minor incident and a true medical emergency.
This article explores what happens when a dog is stung by a bee, the steps to take immediately afterward, and how you can prevent future stings. By knowing the warning signs and treatments, you’ll feel empowered to protect your four-legged friend.
Why Bee Stings Affect Dogs Differently
When a dog is stung by a bee, the bee’s venom enters the dog’s skin through a tiny stinger. This venom contains proteins that can cause pain, inflammation, and in some cases, trigger the immune system to overreact. Dogs tend to get stung on their paws, faces, or noses because of their curious nature — sniffing flowers, pawing at buzzing insects, or playing outside.
The reaction depends on several factors:
-
Location of the sting – The mouth, throat, or around the eyes can be more dangerous.
-
Size and age of the dog – Smaller dogs may react more severely.
-
Sensitivity or allergies – Some dogs are more prone to allergic reactions than others.
Being alert to these factors helps you assess the seriousness of the situation.
Signs Your Dog Was Stung by a Bee
Not all bee stings look dramatic at first. Recognizing the symptoms early is crucial. Common signs include:
-
Sudden yelp or whimper followed by pawing or licking at a spot.
-
Redness, swelling, or a small raised bump at the sting site.
-
Scratching or rubbing the affected area.
-
Localized pain or tenderness.
More serious reactions can include:
-
Facial swelling or hives spreading across the body.
-
Difficulty breathing or excessive drooling.
-
Vomiting, diarrhea, or collapse (signs of anaphylaxis).
If you notice severe reactions, treat it as a veterinary emergency.
Immediate Steps When a Dog Is Stung by a Bee
When your dog is stung by a bee, taking quick action can relieve discomfort and prevent complications:
-
Stay calm and move your dog away from the area.
Bees often sting in groups. Remove your dog from flowers or hives to prevent more stings. -
Locate and remove the stinger.
If the stinger is visible (a small black dot with a sac), scrape it off with a credit card or dull knife edge. Avoid squeezing it — that can release more venom. -
Apply a cold compress.
Use a clean cloth or ice pack wrapped in a towel for 5–10 minutes to reduce swelling. -
Soothe the area.
A paste of baking soda and water or a pet-safe topical treatment can neutralize venom and ease irritation. -
Monitor your dog closely.
Keep an eye out for worsening symptoms over the next few hours, especially difficulty breathing or severe swelling.
When to Call the Vet
Not every dog stung by bee incident requires a veterinary visit, but knowing when to call a professional can save your dog’s life.
Seek immediate veterinary attention if:
-
Your dog is stung multiple times.
-
The sting is inside the mouth, throat, or near the eyes.
-
Your dog shows any sign of allergic reaction (facial swelling, vomiting, trouble breathing).
-
Your dog is very young, very old, or has pre-existing health conditions.
Your veterinarian may administer antihistamines, steroids, or epinephrine in severe cases. They can also provide guidance on at-home care tailored to your dog’s weight and health history.
At-Home Care After a Bee Sting
Once the initial emergency has passed, you can help your dog recover with gentle care:
-
Keep the area clean and dry to prevent infection.
-
Use an Elizabethan collar (cone) if your dog keeps licking or scratching the sting.
-
Offer plenty of water and a quiet resting spot.
-
Follow any medication instructions your vet provides, such as antihistamines or pain relievers.
Most dogs recover within 24–48 hours with proper care.
Preventing Future Bee Stings
While you can’t eliminate all risks, there are steps to reduce the chances of your dog being stung by a bee again:
-
Monitor outdoor play.
Avoid letting your dog roam near beehives, flowering plants in full bloom, or areas with heavy insect activity. -
Trim your lawn and garden.
Bees are attracted to tall grass and flowering weeds. Regular maintenance can reduce bee presence. -
Use pet-safe insect repellents.
Never use human bug sprays on dogs, but some pet-specific repellents can discourage insects. -
Train your dog to “leave it.”
Teaching this command helps your dog avoid pawing or snapping at bees and other insects.
Understanding Allergic Reactions in Dogs
A single sting might be minor, but repeated stings can sensitize your dog’s immune system, leading to stronger reactions in the future. Talk to your vet about:
-
Allergy testing if your dog has reacted severely.
-
Emergency kits for allergic dogs, such as epinephrine injectors.
-
Preventive strategies if you live in areas with high bee populations.
The Emotional Side of Pet Emergencies
When a dog is stung by a bee, it’s not just the dog who’s frightened — owners are too. Staying calm is key. Your dog looks to you for reassurance, and your quick thinking can reduce stress and improve outcomes. Keep your veterinarian’s number handy and know the location of the nearest emergency clinic.
Looking Ahead: Empowered Pet Ownership
Bee stings are part of life outdoors, but they don’t have to be a disaster. By understanding the risks, recognizing the symptoms, and acting quickly, you can protect your pet from harm. The phrase “dog stung by bee” doesn’t have to conjure panic — it can instead be a prompt for preparedness and responsible pet care.
As pet parents become more proactive about their animals’ health, we’re seeing a shift toward better education, faster emergency responses, and preventive measures. Just as modern business leaders blend strategy with social good, modern pet owners blend love with informed action, ensuring their pets’ safety and wellbeing.
Key Takeaways
-
A dog stung by a bee can experience anything from mild irritation to life-threatening reactions.
-
Act immediately: remove the stinger, apply a cold compress, and watch for allergic signs.
-
Contact a veterinarian for severe or multiple stings.
-
Prevent future incidents with smart outdoor habits and training.
Knowing what to do in advance can save precious time and help your furry companion recover quickly.
-

 BLOG1 year ago
BLOG1 year agoSlothokiturbo.net: Exploring the World of Online Gaming and Community
-

 TECH10 months ago
TECH10 months agoHow Cyber Security Services Help Organizations Manage Cyber Risk
-

 BLOG10 months ago
BLOG10 months agoLiteroticatags: Exploring the World of Erotica and Its Online Community
-

 BLOG1 year ago
BLOG1 year agoErothtos: Understanding Its Role in Today’s World 2025
-

 BLOG1 year ago
BLOG1 year agoLeah Gettens: Everything You Need To Know
-

 BLOG1 year ago
BLOG1 year agoWatchmenontheall Calvin: An Exploration of Themes, Characters, and Significance
-

 TECH1 year ago
TECH1 year agoMansrufer: Pioneering Progress in Technology
-

 BLOG1 year ago
BLOG1 year agoUse 1.5f8-p1uzt – A Comprehensive Guide!
